April 17, 2021 ✒ Andrew Kantor
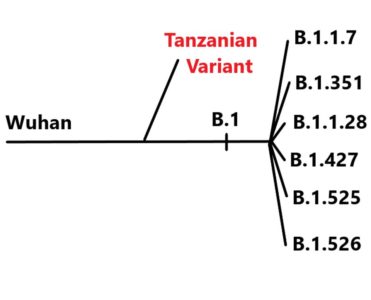
Not entirely surprisingly, there’s a good chance folks who got the Pfizer/BioNTech vaccine will need a booster — a third shot in a year. So says the company’s CEO. This is actually good news. It means that Pfizer is confident that its mRNA technology can be used for boosters to protect against the variants that are emerging. Speaking of which… A new and different beastie. Unlike what we’ve seen so far in variants like B.1.1.7 (“the UK variant”) this one comes from an entirely different strain. It’s an ‘A’ variant. It’s he first of its kind. All your variant questions answered. Finally, while we’re on the subject, you may have questions. The New York Times has most of the answers. … is GPhA’s Spring Region Meeting: April 22, from 7:00-8:00 p.m., virtually (hopefully the last time) via Zoom. Head to GPhA.org/region-meeting and sign up now! If you’ve ever seen a teenager feed, it can be a wonder to behold. Often it’s a just faint whooshing sound … and the box of doughnuts is gone. That’s basal metabolism for ya. But what if you could replicate that in, say, fat mice? And what if you could use an existing drug to do it? Guess what? Digoxin — you know, the heart-disease drug — seems to have an unexpected effect. It cuts the body’s production of interleukin 17, and by doing so reins in inflammation. That somehow increases basal metabolism and burns the weight away. Or, put another way, it let fat mice continue to eat all they wanted, but… These overweight mice soon obtained the same weight as healthy control mice on regular diets, with no negative side effects and the benefits observed for at least eight months. Put another way: Take digoxin, get a teenager’s metabolism, eat all you want, lose weight. Enjoy it while you can Dental care is pretty much the same across modern countries (jokes about the British aside). And yet — found a study by an international team of researchers — dentists in the U.S. prescribe antibiotics more than those in any other country. In, fact, U.S. dentists prescribe them more than twice as often as their Australian counterparts. Why the difference? Are American infections more common than those in Australia? Not likely. The researchers said the different rates did not seem to be explained by differences in dental health, but may be related to differences in the prophylactic use of dental antibiotics aiming to protect people at risk for distance site infections during operative dental procedures. Perhaps, they suggest, an antibiotic stewardship program is in order. A group of U.S. and Chinese researchers have created human-monkey chimeras: They injected six-day-old monkey embryos with human stem cells, and the result lived for about 20 days. Eventually they hope to have the monkeys-with-some-human-cells live longer, so they can “serve as helpful models for human disease, embryonic development and aging.” The idea is that, rather than experiment on humans directly, we could experiment on monkeys with human genes, which is ethically less questionable. Right? And yes, the Simpsons have done it. Computers, say Canadian researchers, can predict whether someone with a psychiatric disorder is likely to commit a crime — and can do it better than humans. And there is nothing whatsoever creepy about this quote: “Knowing the type of crime an individual is likely to commit, before the offense occurs, is urgently needed in order to guide more targeted and precise risk assessment strategies and frontline therapeutic interventions.” A new kind of variant, feed like a teen, the monkey-man chronicles, and more
Three times the charm?
Variant updates
Don’t forget this coming Thursday…
Eat, eat, and be merry

U.S. dentists are enthusiastic about antibiotics
And on the seventh day
None dare call it “precrime”

April 16, 2021 ✒ Andrew Kantor
Cancer patients in Georgia are about to start feeling the effects of “white bagging” (Georgia Health News explains), where insurers use their own pharmacies to deliver specialty drugs, rather than letting hospitals buy them. Anthem Blue Cross and Blue Shield, Georgia’s largest health insurer, is requiring that oncology infusion drugs for its patients be purchased through CVS Specialty, or through the insurer’s own specialty drug network that has similar pricing. There will be similar restrictions on other infusion/injection drugs. And the staff pharmacist, the one who would make sure the dose matches the patient? Don’t worry — the insurance company will take care of that! FDA created a program to approve drugs so old they were created before the agency existed. The idea was to be sure they were safe. The result, though, was that companies branded them and jacked up the prices, making previously affordable medications a lot less affordable. (Colchicine, used for gout for more than 200 years, was about 10¢ a pill until URL Pharma debuted Colcrys — identical but $4.50 a pill.) Hospital executives are particularly vexed about the price hike for Vasostrict — formerly known as vasopressin and first developed in 1928 — because that drug, used to increase a patient’s blood pressure, has been widely used in intensive care units to treat covid-19 patients. From 2019 to 2020, hospital spending for the drug rose 56%, to nearly $600 million, according to the American Society of Health-System Pharmacists. The Biden administration’s short list of candidates is expanding as pressure mounts to make a permanent pick. While Janet Woodcock, M.D., the interim commissioner since Biden took office in January, remains in the running for the permanent job, some politicians and advocacy groups have pushed back on her potential nomination over concerns about past opioid approvals under her watch. Opioid deaths have soared during the pandemic — hitting a record (more than 87,000 Americans in 12 months) and rising 29 percent over the previous year. So figure to pick up this plot thread as the current season winds down. Many treatment programs closed during that time, at least temporarily, and “drop-in centers” that provide support, clean syringes and naloxone, the lifesaving medication that reverses overdoses, cut back services that in many cases have yet to be fully restored. So let’s say you catch Covid, and you don’t want to die. That’s the time to be thinking, “Maybe I should have brushed more often.” A study out of McGill University found that bad oral hygiene was linked to bad Covid outcomes. Covid-19 patients with gum disease were 3.5 times more likely to be admitted to the intensive care unit, 4.5 times more likely to need a ventilator, and 8.8 times more likely to die when comparing to those without gum disease. Oh no, baby — he’s doomed A Boston University study found a shocker: “States that required people to mask up last year had lower rates of Covid-19 than those with no mask requirements.” “This protective effect of mask wearing was evident across four months of the pandemic, even after adjusting the associations for mask policy, distance policy and demographic factors.” Biguanides like metformin are getting new life these days, as researchers find new uses for them. The latest: Phenformin — potent but discontinued as a diabetes treatment — may work as an adjunct with some of the hot new cancer immunotherapies. Right now it’s all pre-clinical experiments, but it seems that phenformin’s potency may be to its advantage. That makes it better at helping those drugs (e.g., BRAF inhibitors) fight tumors. And what about phenformin’s side effects? Still better than chemotherapy’s. “The viral ghost of long Covid” from Vox. You’ve heard of “long Covid,” but “long” diseases are nothing new (looking at you, measles). In fact, long Covid is finally bringing attention to the millions of people suffering from other “medically unexplained” symptoms long after they’ve had a disease. (Not a podcast listeners? Here’s the article in words.) Yet another study (this one in London) has found that psilocybin is an effective treatment for depression. In this case it was compared to the SSRI escitalopram, and did pretty darned well. Small and interesting caveat: Psilocybin needs to be combined with psychotherapy; the idea is that the drug helps bring issues to the surface, which can then be worked out professionally. “With a psychedelic it is more about a release of thought and feeling that, when guided with psychotherapy, produces positive outcomes.” […P]articipants given psilocybin had often reported feeling they had got more fully to the root of why they were depressed.Shroom power, “white bagging,” dirty-mouth dangers, and more
“White bagging” in Georgia
The best-laid plans
FDA commish still up in the air
Two steps back
Brush your teeth

Captain Obvious is smiling (but you can’t see it)
Phenformin vs cancer
Podcast of the week: Diseases that don’t go away
ICYMI: Latest magic mushroom news
April 15, 2021 ✒ Andrew Kantor
Back on April 2 we told you how there’s both an N95 shortage in hospitals, and an N95 glut in warehouses. The basic reasons: Small hospitals are low on cash, larger hospitals’ buyers are wary of buying from companies they aren’t familiar with, so millions of NIOSH-approved masks sit in boxes. Now the feds are changing their policies, and the changes are going to mean more masks demand. Hopefully those smaller, U.S.-based businesses will supply them. America has set another record for STDs, with cases of chlamydia, gonorrhea, and syphilis hitting a new high in 2019 — the sixth year in a row, according to the CDC. (Expect a dip in 2020, though, as people avoided getting tested, then a ‘catch-up’ effect in 2021.) At this point, what doesn’t show promise as a coronavirus treatment or preventative? New on the list — thanks to some presumably very chill Israeli researchers — is cannabis. Well, a “combination of compounds found in cannabis,” specifically some 30 terpenes, e.g., beta-caryophyllene, citral, and eucalyptol. In the lab, at least, they “exhibited an antiviral effect.” Kudos to the Forbes reporter who asked the important question: Can it be inhaled? “It’d be great if we could just sort of smoke our way out of a coronavirus, but I don’t think that this study shows that.” Looking at data from 1999 to 2017, pharmacy researchers at the University at Buffalo discovered that prescriptions for drugs that can increase falls in seniors are going up … and, not surprisingly, so are the number of falls. People receiving at least one potentially fall-increasing drug: 57% in 1999; 94% in 2017. Increase in age-adjusted mortality due to falls from 1999 to 2017: 115% Sayeth the lead researcher: “Our hope is it will start more conversations on health care teams about the pros and cons of medications prescribed for vulnerable populations.” Those shifty Danes have created a new kind of birth control — an alternative to hormones and barriers that’s based on … mucus. They say it’s as effective as the Pill. It works by simply reinforcing the natural mucus barrier in the cervix to make it impenetrable to sperm — thereby preventing sperm from passing through the cervix and fertilizing an egg, minutes after application. Well, not just mucus. There’s a biopolymer involved, too, one “derived from either mushrooms or the shell of crustaceans” because it’s biodegradable and non-toxic — not to mention already in use in medical devices. In animal studies, it’s 100 percent effective. Bonus: Includes phrases like “mucus-centric contraception” and “pre-seed financing.” What causes them? How frequent are they? How dangerous? On a scale from “going back to sleep” to “running in circles screaming,” how worried should you be? Forbes’s Leah Rosenbaum tackles it all: “Here’s What Scientists Know About Covid-19 Vaccine Blood Clots”. Who among us hasn’t had a fat mouse with liver disease? Good news out of Penn State, though — slipping the mice some cocoa powder “markedly reduced the severity of their condition.” [C]ocoa-treated mice gained weight at a 21% lower rate and had smaller spleen weights — indicating less inflammation — than the high-fat-fed control mice. [They also had] 28% less fat in their livers than the control mice […] 56% lower levels of oxidative stress, and 75% lower levels of DNA damage in the liver. So would it work for humans? The researchers think so, but it would require the equivalent of five cups of hot cocoa a day. As part of the rollback of Trump-administration health policies, the FDA has lifted the requirement that mifepristone be dispensed in person, and the White House said it would reverse the “Title X Gag Rule”.Snot your old-fashioned contraception, new STD record, chocolated mice, and more
Mask rule changes a-comin’
We did it again!
Sure, why not pot?
Older folks are falling down, falling down
You had as at “mucus”
Everything you wanted to know about vaccine blood clots
If you give a mouse some cocoa…
ICYMI
April 14, 2021 ✒ Andrew Kantor
Blood type: Despite earlier suggestions, it seems that blood type does not make someone more susceptible to Covid-19. (It’s based on a study of 107,796 individuals, so it would seem to have some weight.) Good and bad: The UK variant — B.1.1.7 to its friends — is apparently more virulent than the basic strain of SARS-CoV-19, but not more severe. So that’s a bit of good news. Winter is coming: The University of Washington’s Institute for Health Metrics and Evaluation (IHME) says to expect a good summer … but a bad winter. The forecast calls for a ‘considerable surge’ of Covid-19 cases “because the new variants are more transmissible, and people will likely relax social distancing and mask wearing.” There’s another new variant, this one in Oregon. It’s kind of like B.1.1.7 Plus, with the “plus” being an additional six mutations… …one in the spike protein, three on the replication complex (ORF1ab), one in the structural protein N, and one in the accessory protein ORF8. There’s not enough information yet, but William Haseltine knows his stuff, and he thinks it’s probably not a friendly variant — it’s one likely “associated with an increased transmission and vaccine resistance.” That’s too long to wait. NOW is the time to register for the 2021 Georgia Pharmacy Convention. If you read this and thought, “Oh, yeah, I’ve got to do that” — don’t wait any longer. Click here to go to GPhAConvention.com and sign up now. The room block’s been open since March 1, and the longer you wait, the greater your risk of ending up in that one wing with the lizard infestation. (Kidding!)(Probably!) Go! Register for the biggest event of the year on the amazing Amelia Island! Do you work for Wellstar? You might want to casually slip that into conversation — after all, Fortune named it one of the 100 best companies to work for. (It’s #90, if you must know.) Wellstar took a major financial hit […] But the health system took aggressive steps to protect the interests of its workers, including by deploying $2.9 million in childcare support for its workforce and pay continuation programs for staffers who were unable to work, as well as more than $2.2 million dedicated to a free meals program. Its CEO Candice Saunders also took a 60% pay cut in an effort to lead by example. Who else is on the list? Publix, Target, and Wegman’s — and, of course, the Cheesecake Factory. “New research,” says Kings College London, “reveals why some of us are hungry all the time.” The shocking reason? Some people’s blood sugar regularly dips low. (Bonus: The college refers to these people as “Big dippers.”) Pharmaceutical companies are freaking out as the Democrats pick up where the Trump administration left off: They also want to either tie when Medicare pays for drugs to what the rest of the world pays, or at least allow Medicare to negotiate prices — you know, basic capitalism. Drug companies, of course, want to keep the status quo, where there is no negotiation: They set the price, and Medicare forks it over. And they’re planning to use the same, tired arguments: ‘It will hurt innovation,’ ‘it will hurt jobs,’ yada yada yada. Since 2015, the FDA has approved 29 biosimilar products, but they’re still not in wide use — unlike generic drugs. What’s up with that? Insurance companies, in large part. They have formularies, and while they rarely care which generic drug a patient takes, when it comes to physician-administered biosimilars, they get picky. And since 2019, larger insurers’ formularies specify which ones they will cover. Think of the poor hospital pharmacist, who has to track multiple virtually identical drugs and which patients get which version. Oh, and insurers change their formularies month to month. Hospital providers can now face a dizzying set of rules that must be carefully tracked when treating patients with different insurers. […] Rather than stocking one or two versions of a drug with no clinically meaningful differences and administering them to all patients, hospital pharmacies must inventory several versions depending on insurers’ preferences that month. Yet more groundbreaking research, this from the University of British Columbia. Mechanical engineers there did the study, and they’re cautioning pregnant women to drive slowly* over speed bumps. And there’s not a bit of hyperbole in this language: If driven over quickly, they caution this can lead to minor injuries to the fetal brain, cause an abnormal fetal heart rate, abdominal pain, uterine contraction, increasing uterine activity and further complications. The FDA wants to “pause” the Johnson & Johnson one-shot vaccine while it investigates reports of fears of blood clots. (Yes, that’s correct — just like with the AstraZeneca vaccine, there have been scattered reports of blood clots with the J&J shot.) The Georgia DPH is doing just that. To be clear: There have been six reports out of the 7,000,000 J&J shots in the U.S. That’s literally more than one in a million. (One in 1.167 million in fact.)Speed bumps of doom, Wellstar gets a thumbs up, PhRMA freakout, and more
Covid quickies
* …which we’re not supposed to call “the UK variant,” because we’re trying to get away from ‘place’ names like “Spanish fly” and “Russian roulette”
And the slightly bigger Covid news
Christmas is 255 days away
Wellstar’s a great place to work
Groundbreaking research
The traffic is tired of bearing
The biosimilars roadblock
Bad baby bump
* Preferably no more than 15.5 mph.
ICYMI: J&J vaccine
April 13, 2021 ✒ Andrew Kantor
The Pfizer/BioNTech vaccine is ready for younger teens, the companies say. Remember, 99 percent effective isn’t the same as 100 percent effective. Long Covid might be more common than originally thought (one in seven have it after three months). Wondering about nasal vaccines? Five of them are in the works; here’s the overview from Smithsonian. Scottish researchers figured out that areas with more sunlight have fewer Covid-19 deaths. But what is it about the sun, exactly? Do the UVA rays just kill more of the virus? Or… “[S]unlight exposure causes the skin to release nitric oxide. This may reduce the ability of SARS Coronavirus2 —the cause of Covid-19 — to replicate, as has been found in some lab studies.” Classrooms are dark, dreary, and probably not as well-ventilated as they oughta be. The beach, though, that’s the place to take a course, right? Even better, there’s no dress code! How convenient, then, that GPhA is offering “APhA’s Pharmacy-Based Immunization certificate training” on Sunday, June 20 — at the beach on Amelia Island! It’s in the same location as the Georgia Pharmacy Convention (again, how convenient!), but it’s a separate registration. If you’re at the convention, why not register for this awesome immunization training? Click here or go to GPhA.org/immunization-2021 — and don’t forget to register for the convention, too! Georgia was ranked the #3 state for working from home by WalletHub — only Delaware and North Carolina were better. In fact, it ranked #1 for “Living Environment” — basically the cost and availability of housing and utilities, including high-speed Internet. The worst states for telecommuting? Alaska, Hawai’i, and North Dakota. Don’t panic, but keep in mind that the pandemic isn’t over — it’s still a race between vaccinations and variants, with anti-vaxxers helping the enemy. If the wrong variant gets a foothold … well, remember how much fun 2020 was? The latest real-world data shows that “The Pfizer/BioNTech Covid-19 Vaccine Is Less Effective Against The South African And UK Variants Than Against The Original Virus”: [T]he vaccine was eight times more protective against the wild type than the B1.351 variant. Similar studies showed that the vaccine is about 2.5 times more effective against the wild type than it is against the B 1.1.7 (UK) variant. Oh, and by the way, the number of Covid-19 cases in the U.S. has been rising each of past three weeks. Could be a lot. Telling a patient he has “hypertension” or has “high normal” blood pressure can do more harm than good. How? Because … psychology. It seems (Aussie researchers found) that those words are strong enough to give people stress, but not strong enough to actually get them to do anything about it. In fact, it may make them put their fingers in their ears and yell “La la la la la la.” “Advising people that they are hypertensive or high normal when they have low risk of cardiovascular disease potentially may cause harm rather than engage them.” (Although it’s worth noting that calling it “hypertension” at least increased their willingness to accept BP-lowering medication.) So what should you do? Read the story for the researchers’ suggestion. If you’ve been wondering if the creating of the mRNA Covid-19 vaccines might foretell the future of the flu shot, you’re not alone. The answer is yes, for sure. It won’t be as fast, though, in large part because flu shots aren’t having billions of dollars (and euros, and yuan, and rubles…) thrown at them. Once it’s cracked, even if we still need one every year, development will be a lot faster. And researchers are talking about the first mRNA flu vaccines coming out within a few years. British researchers have found what could be a huge new treatment for aggressive glioblastoma brain cancers. It’s only in early trials (10 patients), but it seems that a new drug called ipatasertib (an AKT inhibitor from Roche) effectively ‘de-cloaks’ tumors, allowing atezolizumab (the cancer drug) to attack it. “We believe that our findings open the door to the further development of what could become a gamechanging treatment option for some patients with aggressive glioblastoma brain cancer.” The folks at the University of Minnesota have identified “six unhealthy eating behaviors” that have emerged during the pandemic. Well, it’s really five. And even five is stretching it. There’s eating more (mindlessly, eating to cope, and just eating more overall), and there’s eating less (decreased appetite or deliberately cutting food intake for economic reasons). Which ones are you? The official list: And then they count as #6 (?) the fact that there are more eating disorders showing up. The latest example of ‘folk remedies that work’ comes from the Baltic, where amber is the thing: Even today, infants are given amber necklaces that they chew to relieve teething pain, and people put pulverized amber in elixirs and ointments for its purported anti-inflammatory and anti-infective properties So University of Minnesota medicinal chemists wondered what was up. It turns out that yes, Baltic amber does contain ingredients “that show activity against gram-positive, antibiotic-resistant bacteria.” And if you just have to check out the details, those compounds are abietic acid, dehydroabietic acid, and palustric acid.Good news about the sun, five Covid eating issues, hypertension language choices, and more
Covid quickies
Sunny day, keeping the Covid away…
Why not learn to immunize at the beach?
Stay home in Georgia
Yeah, you probably should worry a bit
What you do know can hurt you
The future of flu shots?
Opening the door to brain tumors
Five for eating
Amber alert (no, not that kind)
April 10, 2021 ✒ Andrew Kantor
More than 450 PCOM students — including, most importantly, student pharmacists — spent four days helping vaccinate 1,200 employees in the Newton County School System. Kelsey and Kanan Having sinusitis appears to affect more than the sinuses — University of Washington researchers have found that it also affects the brain, leading to trouble focusing, depression, and other neurobiological symptoms. Or as the school put it: New research links sinus inflammation with alterations in brain activity, specifically with the neural networks that modulate cognition, introspection and response to external stimuli. fMRI scans revealed changes in connectivity in various brain areas, including the frontoparietal network (“executive function, maintaining attention and problem-solving”) the default-mode network (“self-reference […] and mind-wandering”) and the salience network (“communication and social behavior”) Treat Covid with ruxolitinib — meh. But Purdue biochemists found that Covid messes with the lungs in an unexpected way — it “causes expression of an activated complement system,” which usually happens in the liver. By combining ruxolitinib (to target the complement response) with remdesivir (to fight the virus) you get a potential powerful treatment. Do not take an animal de-worming drug — ivermectin — to treat Covid-19. So say health officials. Really, though, do you need “health officials” to tell you that? Yet — with a roll of the eyes, I’m sure — NIH scientists will test whether human ivermectin can treat Covid symptoms. (Kudos to them, really, because who would have thought bread mold could treat infections?) “It’s like the new hydroxychloroquine,” said Angela Rasmussen, a virologist at Georgetown University’s Center for Global Health Science and Security. “It would be great if ivermectin did work — it’s been around for years and is cheap. But to my knowledge, there is no data that suggests it’s good for Covid-19.” The sheep on the bottle should be a clue “Toenail fungus medication may also protect against COVID-19” — and that’s from actual researchers in Germany. Researchers from the University of Muenster say the antifungal drug itraconazole (or Snoporax) killed the deadly bug in experiments. The antidepressant fluoxetine (Prozac) had the same effect, but worked best in conjunction with the more common coronavirus treatment remdesivir. Marvel and the FDA have teamed up to create a comic about the dangers of addiction — vaping, in particular. Honestly, what more is there to say. You can read it on Marvel.com or watch the 8:24 video. After a tumor has been removed, there can still be rogue cancer cells milling about. Now Japanese researchers have developed a hydrogel that can carry a medication to the site. But that’s not a big deal. These hydrogels protect the medication from breaking down. Also not news. They can release those meds based on a change in the tumor site — temperature, pH, etc. Cool, but still not that new. What’s new is that these hydrogels can be designed to respond to a variety of conditions, meaning they could conceivably release different meds depending on what’s going on at the site — temperature, pH, or oxygen concentration. For instance, when conditions are just the right level of acidic in the tumor microenvironment, these DDSs [drug delivery systems] either shrink or swell and release the drug. A NASEM (National Academies of Sciences, Engineering, and Medicine) committee has determined that using human stem cells to create “tiny brainlike structures” doesn’t violate ethical guidelines … or, presumably, have philosophical implications. [T]he committee concluded organoids aren’t capable of consciousness because they lack the many cell types and connected structures of a brain. Even recent organoid experiments that claimed to detect brain waves similar to those in a fetus found “relatively nonspecific” signals — the panel didn’t find this work ethically troublesome. Also: Transplanting human cells into animal brains also gets the thumbs up.Don’t deworm yourself, the toenail fungus solution, not the Avengers, and more
PCOM, represent!

From nose to brain
Greater than the sum of its parts
Oh, sheesh, this again?

All that said…
Age of Juul

Hydrogel 2.0
Growing brains is apparently ethical
April 09, 2021 ✒ Andrew Kantor
The latest on Georgia’s Covid-19 response, courtesy of the amazing Amber Schmidtke: We’re doing much better when it comes to new cases and test positivity, and not too bad for hospital admissions. Where the state needs work is the death rate (worst in the nation), and getting more vaccines into arms — although we’re starting to catch up: Give us a quick hand, would you? Please take this eight-question, two-minute* survey about why you’re a GPhA member. We want to understand you better — thanks! (Sadly, “So I can get GPhA Buzz” is not one of the choices.) Everyone’s expected to multitask these days, so why not sutures? Yeah, the little filaments used to hold wounds closed. While they’re sitting there, they could do a bit more, dontcha think? McGill University researchers thought so, so they’ve developed a 21st-century suture. First, it’s soft — covered in “a slippery, yet tough gel envelope.” But even better, these new sutures can include drugs and sensors — “loaded up with antibacterial compounds, pH-sensing microparticles, drugs and fluorescent nanoparticles” — to help wounds heal. It’s like a “person of interest” when it comes to cancer — “NLRP3.” Normally, it’s a mild-mannered receptor that looks for pathogens. When it’s in melanoma, though, it gets a little wild, and it can help the tumor grow. That’s what University of Colorado researchers found, and more importantly, “By inhibiting NLRP3, the researchers found, they can reduce inflammation and the resultant tumor expansion.” What’s nice about this is that it’s yet another new target in the fight against cancer, and we seem to be uncovering a lot of those lately. The latest government figures show that “More than 528,000 Americans have signed up for Affordable Care Act coverage on the federal exchange in the first six weeks of the special enrollment period.” That’s double the number of signups in the previous two years. Open enrollment through Healthcare.gov is available until August 15. What happens when neuroscientists are up late at night, staring at the stars, coming up with experiments? This happens: “Scientists Have Induced Hallucination-Like States in Mice to Study Psychosis” — which is exactly what it says on the tin. They forced the mice to play a “game” in which the mice would indicate whether they heard a sound that was obscured by noise. Playing the sound more frequently made the mice hallucinate that they had heard it. Then they gave the mice ketamine. Not surprisingly, “Mice that were given ketamine before performing the task also reported more hallucination-like events.” What’s the point? “[It] enables us to finally probe the neurobiological roots of this mysterious experience.” No, it doesn’t involve watching the first 10 minutes of “Up.” This one’s a blood test, developed at Indiana University. Essentially, psychiatric researchers tested the blood of hundreds people with depression over four years. They were able to identify a group of biomarkers that changed depending on how depressed they were. The result is a test that looks for levels of several RNA biomarkers “that can distinguish how severe a patient’s depression is, the risk of them developing severe depression in the future, and the risk of future bipolar disorder.” An gaming app being used to treat ADHD — EndeavorRx — is being tested to see if it can help people experiencing the brain fog of long-haul Covid-19 patients. The game challenges the player’s focus and multitasking by having them navigate a freakishly colorful character through a course, collecting targets, and avoiding obstacles” — kind of like life. It’s supposed to “target areas of the brain that play a key role in attention function.” Willy Wonka, eat your heart out The hope is that it can improve their brain function … and possibly be used to treat other cognitive disorders. Gilead’s triple-negative breast cancer drug has been given the thumbs-up by the FDA. It’s the ninth antibody-drug conjugate drug on the market and the first for triple-neg breast cancer. (Want to know about the other eight? There’s a website dedicated to ADCs.) Not a huge deal, but take note: A-S Medication Solutions is recalling 198,350 bottles of extra-strength acetaminophen tablets after bottles were found to include an incomplete prescription drug label, rather than the required over-the-counter drug facts sheet. If you have patients with Humana insurance, these were distributed in a “Health Essentials Kit.”Hallucinating rats, slicker sutures, gaming against the fog, and more
How’s Georgia doing: The good and the “needs improvement”

What’s a nice pharmacist like you doing in a place like this?
* It’s actually about 90 seconds.
Doing more with sutures
Another cancer target
Half a million more
Rat trips
Depression test
Potential Covid-fog treatment: a game

Trodelvy approved
Acetaminophen recalled
April 08, 2021 ✒ Andrew Kantor
Good news for diabetic rats: Researchers in Abu Dhabi have found a way to make an insulin pill where the drug isn’t destroyed by their stomach acids. They did it using nanoparticles (of course), but really cool nanoparticles: They do double duty — not only protecting the insulin from stomach acid, but also releasing that insulin in response to elevated glucose. We’ve known for a while that it takes some people a long time to recover from Covid-19 — even if you aren’t a true “long-hauler,” symptoms can last months. The latest: A huge study in the Lancet (230,000 patients!) reports that one out of three people who “recover” from Covid “suffer from a neurological or psychiatric diagnosis six months on.” The most common conditions were anxiety (17 percent of patients) and mood disorders (14 percent). For 13 percent of patients the disorders were their first diagnosis of a mental health issue. Even without Covid symptoms, kids are being struck by MIS-C, a nasty (and mysterious) respiratory syndrome about three weeks after their coronavirus infection. Every time there’s a spike in Covid cases, three weeks later there’s a spike in MIS-C. The worst part: These kids may not even realize they’ve been sick until their immune system goes haywire. “[M]ost MIS-C illnesses are believed to result from asymptomatic or mild Covid-19” followed by a hyper-inflammatory response that appears to occur when the patients’ bodies have produced their maximum level of antibodies to the virus. Bored of Covid-19? No one blames you. So what’s on deck? A new website called Spillover is where infectious-disease folks are tracking and ranking the next zoonotic viruses likely to jump to humans. Currently at highest risk: Coronavirus 229E (Bat strain) based on the number of species it infects, how widespread potential hosts are, and a bunch of other factors (e.g., “Intimacy of interaction between domestic animals and humans in the host ecosystem”). If you thought pharma companies were paying physicians, get ready for this surprise: “Medical device firms’ payments to doctors far outstripped those from pharma.” Surgical specialists were the ones getting the most, er, thank-you gifts — they “received seven times more money from device firms than [from] drug vendors.” If the relationship between the patient and physician is “contaminated by perverse financial incentives, then it does erode the public trust, which is a sacred value in our heritage, our great medical heritage.” As one oncologist put it, “The companies know where their bread is buttered.” While you can’t say that “gut microbes cause autism,” University of Colorado microbiologists have discovered that changes in gut microbes can affect where someone appears on the spectrum. Not only did they find that people with autism had different microbe compositions than those without, but when the microbes changed, so did behavior: [D]ifference in levels of lethargy/social withdrawal measured in individuals at different time points correlated with the degree of change in gut microbiome composition. The British sort-of equivalent to the FDA — National Institute for Health and Care Excellence (NICE) — has issued new guidance for chronic pain: Maybe cut out the painkillers. Not that patients aren’t in pain. Rather that chronic pains are unique, and painkillers (says NICE) don’t help when it’s chronic: This is because there is little or no evidence that they make any difference to people’s quality of life, pain or psychological distress, but they can cause harm, including possible addiction. Instead, other treatments — including antidepressants and good ol’ exercise — are more likely to help with quality of life. People with severe liver disease often have a “devastating” itching. Duke medical researchers have figured out why. The short version: Patients with liver disease have too much of a particular fat in their blood (lysophosphatidylcholine (LPC), if you must know). And LPC, when it reaches the skin, opens an ion channel called TRPV4, letting calcium ions pour through. Then … well then, science happens, with a signaling cascade, vesicle formation, and micro-RNA. And that causes an itch. “That’s nice,” you say. “So what?” It means a potential treatment for that itch — and other itches. And it shows that the skin is busier than you might think: “This current research is getting us into a more exciting territory of the skin actually moonlighting as a sensory organ.” Congrats to Sonia Sein of New York, the first person to ever undergo a trachea transplant. What’s noteworthy (besides the fact that this was a crazy-tricky operation): Doctors think that there may be more to come, thanks to Covid-19’s ability to damage our entire breathing apparatus.Autism from the gut, insulin from a pill, itching from the liver, and more
Insulin in a pill?
Covid aftereffects
Mental health issues
The kids aren’t all right
Time to register “Covid229E.com”?
“Perverse financial incentives”
Autism gut check
Chronic pain? Keep calm and carry on
More about itching than you expected
The wind in her pipes
April 07, 2021 ✒ Andrew Kantor
What with SARS-CoV-2 not living long on surfaces (at least until a new variant arises) the CDC now says you don’t need to go crazy with the Lysol wipes or the bleach. Good ol’ soap and water will do the trick. “Routine cleaning performed effectively with soap or detergent, at least once per day, can substantially reduce virus levels on surfaces.” Qelbree: It’s not just a colony of the Klingon Empire, it’s also a newly approved ADHD drug. In fact, it’s the first new ADHD drug approved for kids in more than a decade. (Adult testing is underway.) Fun facts: Unlike most ADHD drugs, Qelbree is neither a stimulant nor a controlled substance — nor (despite what you may have heard) is it the name of Elon Musk’s second child. The other day we asked your reaction to the story that pharmacists are doing well thanks to Covid vaccinations — they’re bringing more people into their stores. Shots bring people into pharmacies, where they have to hang out during the 15-minute observation period — creating a big opportunity for sales. What you said: You won’t find quite as many cheerful, optimistic folks as former FDA commish Robert M. Califf or Emory University professor emeritus Nanette K. Wenger. Writing in the journal Circulation, they predict a post-Covid ‘Enormous wave of death and disability’. “[T]he magnitude of destruction will be forever sealed into our collective memories.” Their glass is bone dry CDC: The Pfizer vaccine is best given with three weeks between doses. Walgreens: Well, four weeks makes it easier for us, because calendars. CDC: (polite cough) Walgreens: Fine, fine. Are you still slumming it with plain old ink tattoos? Besides the fact that no one knows what’s in that ink, they’re kind of boring. What you want is one made with gold nanoparticles, acts as a blood sensor, and can change color. Conveniently, that’s just what scientists at Germany’s Johannes Gutenberg University have come up with. (Well, it’s not a tattoo so much as an implantable sensor, but they called it a tattoo so I’m going with it.) The sensor is based on color-stable gold nanoparticles that are modified with receptors for specific molecules. Embedded into an artificial polymeric tissue, the nanogold is implanted under the skin where it reports changes in drug concentrations by changing its color. Cancer cells have a nasty habit of hiding when they sense danger, turning into stem cells, then reemerging when the coast is clear. Attacking those cells with drugs would be great, but they’re sneaky devils and hard to come by. So Japanese researchers found a way to get those cancer stem cells out in the open. They used a hydrogel “made up of a network of two chemicals and a whole lot of water” (aka a “double-network” or “DN” gel). When cancer cells were put into the hydrogel, they freaked out and turned into stem cells — but now they were out in the open where they could be studied. In fact, the team has already “uncovered a few clues about the mechanisms involved in cancer cell reprogramming.” The hope is that this DN gel can be used to further unravel the secrets behind they way cancer cells are reprogrammed and the way cancer stem cells function, which could lead to more effective drugs to take them out. HBO is there for you with its documentary “The Last Cruise” about the voyage and quarantine of the cruise ship Diamond Princess. (You can also read the Atlantic article by passenger Gay Courter, or her book Quarantine!: How I Survived the Diamond Princess Coronavirus Crisis … or just the Wikipedia article. Up to you.) Not melodramatic at all Walgreens counts to three, post-pandemic doom, our poll results, and more
No radio, soap
First new ADHD drug in — squirrel!
Poll results
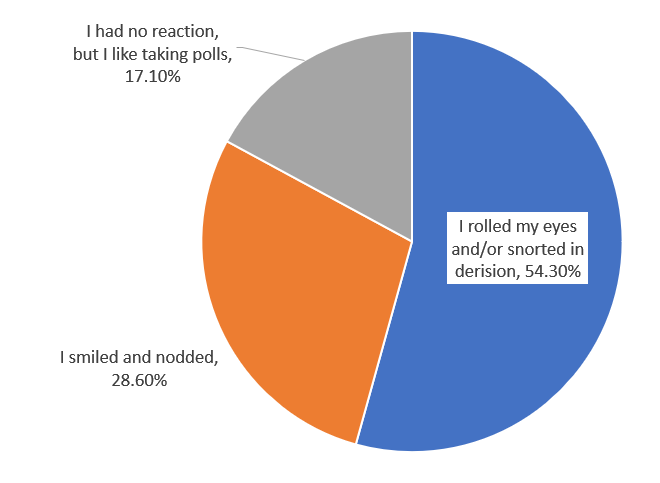
Doctors Doom

The number of the counting shall be three
Tattoo you
And the gel cried out, “No hiding place”
In the mood for a depressing film about Covid-19?

April 06, 2021 ✒ Andrew Kantor
Today I learned: Redheads have different pain sensitivities than normal people. It wasn’t clear, though, why this was true. So Mass General researchers figured to answer the question. What they learned: Redheads have a slightly different kind of pigment-producing skin cell. (It’s the reason gingers don’t tan.) But that same cell variant also secretes lower levels of a molecule called proopiomelanocortin, which breaks down into hormones related to pain. Less proopiomelanocortin, fewer pain-regulating hormones. The presence of these hormones maintains a balance between opioid receptors that inhibit pain and melanocortin 4 receptors that enhance perception of pain. The bottom line: Skin pigment can affect how much pain someone feels. High-five to GPhA board member Ashish Advani, who was featured — along with his company, InpharmD — in the AtlantaINNO business journal. The topic: countering misinformation. “It’s pretty messed up that you can compare the effectiveness or cost of a blender on Amazon, but you can’t do it for a drug,” Advani said. “That’s what we’re building.” We did it — we made it through another legislative session with a good medal for our advocacy team — our big bill passed and awaits the governor’s signature. But there’s more, of course, and Greg Reybold gives the details before taking a well-deserved break*. From vaccine expansion to Covid-19 testing — to what other pharmacy and health bill passed or failed — check out this week’s update. Three types of patients: Looking at more than 7,500 medical records, researchers at the University of Minnesota figured out there are three main types of Covid-19 patients: “The authors conclude that phenotype-specific medical care could improve COVID-19 outcomes.” Hitting our stride: In the course of just the last two months, the U.S. went from lagging most of the world in Covid response to leading it. The latest: We’re giving out more than three million shots per day — well above what we hoped to do. But for how long? Scientists are pretty sure the vaccines give at least six months’ of immunity, but after that it’s anyone’s guess. Which means if too many people remain unvaccinated, we could be caught in a Groundhog Day loop. As if there’s any privacy left: So, um, what are chain pharmacies doing with all the info they collect about people getting a vaccine? “The stores’ online appointment portals usually don’t make explicit how the companies will use the information customers are providing.“ Many of the pharmacies require people to provide at least phone numbers or email addresses at the point of booking an appointment. Some others […] require that people create online user accounts before they can search their websites for still-limited vaccine appointments. A bar in Illinois. About 100 people in it, not one who was vaccinated. “Inconsistent mask wearing and lack of maintaining physical distancing.” How do you think it turned out? (The envelope, please!) The result: At least* 29 people in the bar tested positive for Covid-19 within days (including one person who just got a first vaccine shot). One patron who tested positive was a CNA at a long-term-care facility. One of those 29 also “reported 26 close contacts at a school,” which has so far resulted in two sick student athletes, and the school closing for two weeks. And at least 15 other non-patrons caught it from those 29. British breast cancer patients will be getting a new treatment — a drug combo called Phesgo (pertuzumab and trastuzumab) that’s injected, rather than given via infusions. The treatment takes as little as five minutes to prepare and administer, compared with two infusions that can take up to two and a half hours, NHS England said. Giving glioblastoma patients their chemotherapy in the morning appears to add several months to their lives. Apparently glioblastoma cells have a circadian rhythm of some sort, found Washington University researchers. And with the average life after diagnosis only about 15 months, those would be important months. “These results are exciting because they suggest we can extend survival simply by giving our standard chemotherapy in the morning.” Anabolic steroids (AASs) make some things bigger, some things smaller, and have a range of side effects. Add to that latter list: accelerated brain aging. Norwegian researchers looked at data from about 2,000 guys (aged 18 to 92), figured out what their “brain age” should be, and then looked at what it actually was. Not surprisingly, AAS users had a bigger brain age gap compared to non-users. Those with dependence on AAS, or with a longer history of use, showed accelerated brain aging. The researchers accounted for use of other substances and for depression in the men, which did not explain the difference between the groups. This isn’t surprising; we know steroids affect the brain, especially in Barry Bonds-level doses. What was surprising was how bad this “deviant brain aging” actually was. UGA and Augusta University have partnered to give chemistry students at Augusta a path to meaningful work with their degrees. AU students in their junior year who maintain certain academic criteria and successfully fulfill all admissions requirements will receive a guaranteed admission interview at UGA. Those admitted then can complete their bachelor’s degree with transferred credits earned through the Pharm.D. program. Just a reminder that there’s another story thread we’re going to have to pick up this season: “Drug Overdose Deaths Spiked To 88,000 During The Pandemic*” — that’s up 27 percent from the year before.Redhead pain, which Covid are you?, shrinking steroid brains, and more
Ginger pain
InPharmD shout-out
Legislative update
* Not really. He never sleeps.
Covid quickies
Let’s play “How Do You Think It Turned Out?”
* Not everyone would cooperate with health officials, so the real number is certainly higher.
Quicker breast cancer treatment
First things first
Steroids make brain bad
UGA streamlines pharmacy path for Jags
Overdoses were spiking
* September 2019 to August 2020